
Superovulation with IUI
Unfortunately, most people doing IUI do not follow a very precise technique and the procedure is unnecessarily blamed for the failure. IUI can give the best results only when better quality follicles are produced by gonadotrophin injections, proper ultrasound monitoring is done, proper semen processing is done IUI is done at the correct time, in a correct way and proper support-medicines are given after IUI.
Indications of IUI:
- Patients in whom everything is normal but still there is infertility: unexplained infertility
- Immunological infertility
- Male infertility
- Bad cervical mucous
- Endometriosis
- Unilateral tubal damage
Ovaries can be stimulated to produce ova by tablets-clomiphene citrate-CC, or by injections –gonadotrophins. Gonadotrophins give a much better ova quality than CC. The chances of pregnancy with IUI alone is 2.7 % only, with gonadotrophins only without IUI is 6.7%, but combining the two can increase the pregnancy rates to 26.4% per cycle. Ovarian stimulation can also be done by a combination of CC and gonadotrophins, but results are not as good as that with gonadotrophins alone, though the cost is definitely reduced. There are 3-4 different gonadotrophins available, but rFSH has been proved to be the best worldwide. This is the gonadotrophin which is used in the world’s best centers today.
The advantage of IUI is that a bulk of the best quality sperms are placed in the uterus- closer to the ovum and vaginal acidity is also bypassed, so fertilization is facilitated.
Assessment of follicle quality and endometrial receptivity:
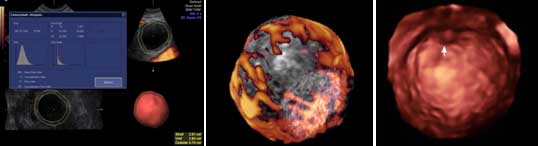
This is done by 2D, Doppler, 3D, and 3D power Doppler ultrasound. When follicle grows to the required size, Doppler is done to assess its functional capacity. When endometrium grows to the desired thickness, its Doppler is also done to assess its implantation capability.
Parameters of a good follicle quality:
- A minimum diameter of 16-18 mm.
- Vascularity covering 3/4th of its circumference.
- These vessels having RI of 0.4-0.48 and PSV of at least 10cms/sec
- The follicular volume of 3-7 cc
- Presence of cumulus oophorus (a cell group in which the actual ovum is protected)
- 3D power Doppler parameters: VI > 8, FI > 27, VFI > 2.

Parameters for a good endometrium:
- At 6 mm, preferably 8-10mm thickness
- Grade A/B endometrium
- Blood vessels reaching the inner layers of the endometrium
- These blood vessels have RI < 0.6
- Uterine artery PI < 3.2.
- Endometrial volume > 3cc
- 3D power Doppler parameters: VI > 30, FI > 40, VFI > 20.


Stimulation is continued till these parameters are achieved and then ovulation trigger is given to rupture the follicle. In patients with polycystic ovarian syndrome(PCOS), there are multiple follicles and if trigger is given, these patients are likely to develop a serious complication called ovarian hyperstimulation syndrome. In these patients, therefore, GnRhagonist is given for trigger. IUI is done 36-38 hours after trigger or GnRha injection. IUI is done with its specialized cannula.
Semen, which is processed in the lab to separate the best quality sperms is used for IUI. This processing can be done by two methods. 1. The swim-up technique, which is used for semen samples with normal count and motility. 2. Gradient method: this is used for semen samples with low count and low motility. For good semen preparation, the laboratory should be equipped with a microscope, CO2 incubator, simple incubator, and a high-quality centrifuge machine. Moreover, each semen sample is different and requires a little modification of technique and so the person doing the semen processing should be specially trained for it and should be a dedicated and sincere worker. A well-prepared sample should have no debris and 95% of sperms in the sample should show good motility.
The time interval for the processed sample, from the CO2 incubator to the patient’s uterus should be the shortest. Therefore it is always preferable that the semen processing lab is on the same premises as the infertility center or where IUI is done. All only disposable ware is used for the processing. No antiseptics are to be used during IUI as it damages the sperms. Any compromise at any of the previously described steps will definitely compromise with the results.


Keys to the success of IUI:
- IUI should not be planned after confirming the rupture of the follicle on ultrasound.
- IUI must be done at 36-38 hours after trigger.
- A sperm count of 4 million after semen processing is considered as optimum but the best results are achieved when the count after processing is 8-10 million.
- A semen sample that is properly processed must have no debris and 95% motility.
- Only 0.3-0.7ml of processed semen samples must be put in the uterus on IUI.
- IUI must be done with a dedicated IUI cannula only.
- After doing IUI patient is allowed to rest for 15 minutes.