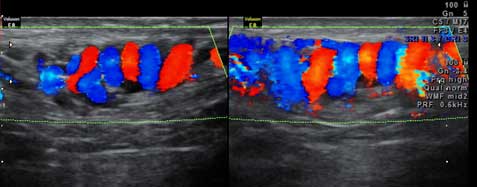
Role of colour Doppler and 3D-4D ultrasound in Infertility and Gynaecology
Transvaginal ultrasound and colour Doppler are inevitable parts for evaluation of any gynaecological or infertility problems in female. It is a single noninvasive test that gives more information than any other test. Two dimensional ultrasound shows the anatomical status of the part examined. Colour Doppler gives idea about the blood flows. Blood flows are reflection of the hormonal and functional status of the organ. Therefore colour Doppler assessment is assessment of physiological status of ovary or uterus, maturity of follicle and receptivity of endometrium. Complete cycle assessment for infertility therefore should consist of transvaginal colour Doppler study which reflects the hormonal changes occurring during the menstrual cycle.
During the first visit of the patient, a first scan is done-pilot scan. This is done to exclude abnormalities of uterus, ovaries and tubes. Transvaginal ultrasound(TVS) is combined with 3D ultrasound to diagnose congenital uterine abnormalities like unicornuate, bicornuate, septate or arcuate uteri. TVS combined with Doppler and 3D ultrasound is the investigation of choice for diagnosis of acquired uterine abnormalities like fibroids, adenomyosis, polyps, synechiea etc. This scan is also done to assess the ovaries for any abnormalities like, cyst, heamorrhagic cyst, chocolate cyst, dermoid, etc and also tubal lesions like hydrosalpinx.
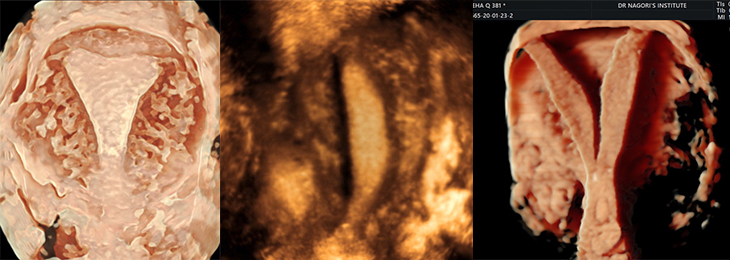

Scan is done on day 2nd or 3rd of the cycle. This is called baseline scan. This scan is done to find out what drugs and what doses will be required to achieve adequate ovarian stimulation. This is important because there are some low reserve ovaries, which would not produce many follicles in spite of high doses of stimulation and there are some polycystic ovaries which would produce multiple follicles even with lower doses for stimulation. Stimulation cycles have to be cancelled in both instances. Therefore stimulation should be started only after doing the baseline scan and deciding the dose according to the findings.
Follicle and endometrial growth in response to these drugs is monitored by ultrasound. When the follicle of 16-18mm is seen, colour Doppler is used to assess the flows surrounding the follicle and in the endometrium to know the functional status of both. If both appear functionally capable, then hCG is given and IUI/IVF may be planned. In spite of doing such a detailed assessment, conception rates are not 100%. That means there is still a chance of improvement. Therefore follicles and endometrium are assessed with 3D and 3D power Doppler ultrasound to be even more precise about the functional capabilities of the follicle and the endometrium. We have done a large study on this nd have found that including 3D and 3D power Doppler parameters in decision making for timing of hCG and IUI/IVF has significantly improved our conception rates. This study was presented first at Annual congress of International society of ultrasound in obstetrics and gynaecology in September 2006 at London.

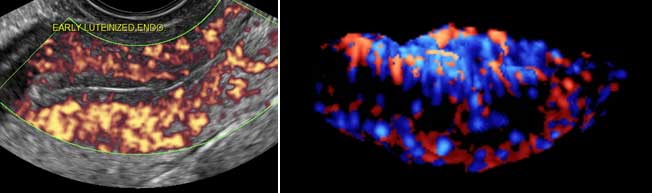
One more scan is also done during the later phase of the cycle, day 22-25, or 7-9 days after IUI. This scan is important to know the abnormalities or deficiencies in this- luteal phase of the cycle, that is after rupture of the follicle. After the follicle ruptures, it is known as corpus luteum. Corpus luteum is responsible for the secretion of the pregnancy supporting hormone-progesterone. It is the colour Doppler study of corpus luteum that gives idea about the adequacy of progesterone secretion. Doppler study of endometrium is also done at this stage to assess, whether progesterone produced by the corpus luteum is adequate for endometrial changes to support the implanting embryo. If it is not further pregnancy support may be given to improve the chances of implantation.
Apart from ultrasound being used for diagnosis of abnormalities of uterus and ovaries and also for cycle assessment, it is also used for assessment of tubal patency and tubal status. This is known as sonosalpingography. Especially in patients on whom laparoscopy is already done once & the tubes are suspected to be blocked, this investigation can be done & more invasive techniques can be avoided. HSG also can be done for the same purpose but this technique has disadvantages of using iodinated dye, which has high risk of reaction, it is very painful & also using X-radiation. Instead sonosalpingography is a much simpler painless & a less time consuming procedure. Moreover it uses only normal saline as a dye, which can be seen coming out of the tubes on sonography and has no risk of reaction.

With the advent of new contrast mode in new machines and availability of ultrasound contrast, assessment of tubes have become much more accurate than what is could be with sonosalpingography. This is called HyCoSy. With this contrast it is possible to see the whole tubal lumen and its fimbrial end and spill of the contrast out from the fimbrial end, similar to that seen on laparoscopy. The condition of the tubal lumen can also be assessed and site of the block can be defined with fair accuracy. But for assessment of tubal status still laparoscopy is the gold standard because tuboovarian relationship can only be assessed by laparoscopy which is very vital for fertility.
Males have dilated veins in the scrotum called varicocoele & is a very common cause of low sperm count/ variable sperm count low motility. Varicocoele can be diagnosed by colour Doppler with confidence. Some males have zero sperm count called For these patients 3D Sonography is done to find out if there is block in any of the tubes which carry the sperms & secretions from testis to the urethra. If one of these tubes show a block, it indicates that the testes are producing sperms & so sperms must be present there but are not carried to the semen. In these patients sperms can be aspirated from the testis and ICSI can be done & they can father a child inspite of their semen sperm count being zero. But if these tubes show no block and still the count is zero, it means that the sperm production in testis is affected and for these patients, there is hardly any option except donor semen from sperm bank for conception. Thus transvaginal colour Doppler & 3D sonography are now indispensable for all gyneac/ infertility patients.